The Vascular Surgery Fellowship Program
The University of Tennessee Graduate School of Medicine Vascular Fellowship Program is an ACMG accredited two-year training program leading to board eligibility for a certification in Vascular Surgery granted by the American Board of Surgery. Our program provides vascular fellows a broad comprehensive experience in all aspects of care for those afflicted with vascular disease. Established 25 years ago, the program has alumni practicing throughout the United States with one third of the graduates active members of academic surgical training programs. The overall first attempt pass rate for both the qualifying and certifying exam is 100% for our graduating fellows over the past five years. The achievements of the program are directly attributable to the dedicated core faculty who are committed to the success of the program as well as the vascular fellows.
The vascular surgery fellowship goals are:
- Attract and educate a diverse set of highly qualified fellows who upon finishing the program will become board certified and be competitive for either academic or private practice positions.
- Provide exemplary vascular care for patients throughout the East Tennessee region.
- Foster a culture of intellectual collaboration in clinical care and basic science research.
- Be recognized for clinical excellence, educational leadership and innovation in vascular treatment both regionally and nationally.
With all patient care occurring on the campus of the University of Tennessee Medical Center (UTMC), the vascular program provides the vascular fellow a high volume of open surgical and endovascular experience during their fellowship. With ancillary support provided by general surgery interns/ residents and mid-level providers, the vascular surgical services train the vascular fellow to be a leader of an efficient patient care team. Moreover, the division's basic science research laboratory led by a full time PhD provides the vascular fellow experience in vascular wall biology and vascular translational research. Finally, the ability to be an active participant in the division's non-invasive vascular laboratory as well as interact with the radiology department residents and faculty provides the vascular fellow an excellent experience in learning and interpreting vascular diagnostic testing.
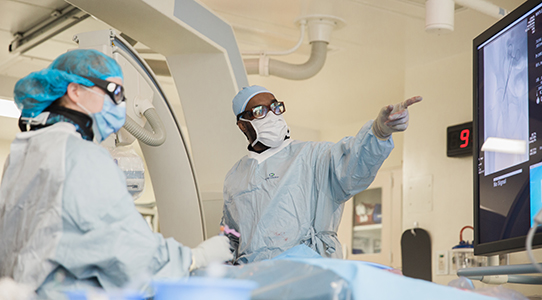 The first year of the vascular surgery fellowship program is spent learning noninvasive vascular imaging, conducting research in the basic science vascular laboratory, rotating on the clinical vascular services, dedicated clinic rotation, as well as learning endovascular skills. The fellow will spend one month in the noninvasive vascular laboratory learning interpretive skills of noninvasive vascular imaging as well as hands on performance of noninvasive vascular studies. Two separate months in the first year (based on the fellow’s choice) will be dedicated to clinical research or basic science research in the Vascular Research Laboratory, which conducts research in vascular wall biology and translational research. During the first research month, first year fellows complete a one week UT GSM instructional course on conducting clinical research. In addition, first year fellows prepare to complete the RPVI exam during these research months. Two months are spent on a dedicated endovascular rotation learning diagnostic and therapeutic endovascular skills. Finally, seven months are spent on traditional clinical vascular surgery services leading their respective resident teams.
The first year of the vascular surgery fellowship program is spent learning noninvasive vascular imaging, conducting research in the basic science vascular laboratory, rotating on the clinical vascular services, dedicated clinic rotation, as well as learning endovascular skills. The fellow will spend one month in the noninvasive vascular laboratory learning interpretive skills of noninvasive vascular imaging as well as hands on performance of noninvasive vascular studies. Two separate months in the first year (based on the fellow’s choice) will be dedicated to clinical research or basic science research in the Vascular Research Laboratory, which conducts research in vascular wall biology and translational research. During the first research month, first year fellows complete a one week UT GSM instructional course on conducting clinical research. In addition, first year fellows prepare to complete the RPVI exam during these research months. Two months are spent on a dedicated endovascular rotation learning diagnostic and therapeutic endovascular skills. Finally, seven months are spent on traditional clinical vascular surgery services leading their respective resident teams.
During the second year, the vascular fellow rotates between the clinical vascular services during which the fellow will see a wide spectrum of vascular diseases under the direction of seven board certified vascular attendings. Inpatient, outpatient, and operative care are under the direction of the vascular fellow with close supervision by the attendings. The graduating fellow can expect to finish with over 500 major vascular cases and total case volumes well above the average national graduating vascular fellow.
In addition to the clinical responsibilities, there is a weekly Vascular Conference, Morbidity and Mortality Conference, Performance Improvement Conference and Research Conference. At the end of the clinical year of the vascular surgery fellowship, the fellow is expected to obtain sufficient preoperative, intraoperative, and postoperative experience to care for patients with peripheral arterial, venous, abdominal, visceral artery, renal artery, thoracic aortic, cerebrovascular and lymphatic disease. It is expected that the resident will take both the certifying and qualifying exam of the American Board of Surgery and pass the RPVI exam.
Application Process
- All applicants should submit through Electronic Residency Application Service (ERAS). Our fellowship program is listed as "University of Tennessee Medical Center at Knoxville" and our program ID is: 4504721075.
- All applicants must participate in the National Resident Matching Program (NRMP).
- Applications must also include:
- Résumé or Curriculum Vitae
- Personal Statement
- Transcript
- ABSITE scores
- Completed Application Form
- USMLE scores
- Three Letters of Recommendation
- Foreign medical school applicants must be ECFMG certified.
- The institution only sponsors J-1 Visas.
- The Department of Surgery does not discriminate on the basis of gender, race, age, religion, color, national origin, disability, veteran status or sexual orientation.
After the applicant has submitted this information through ERAS, the completed application will be reviewed by the Pre-Selection Committee. Interviews for invited residents will take place between January and March.
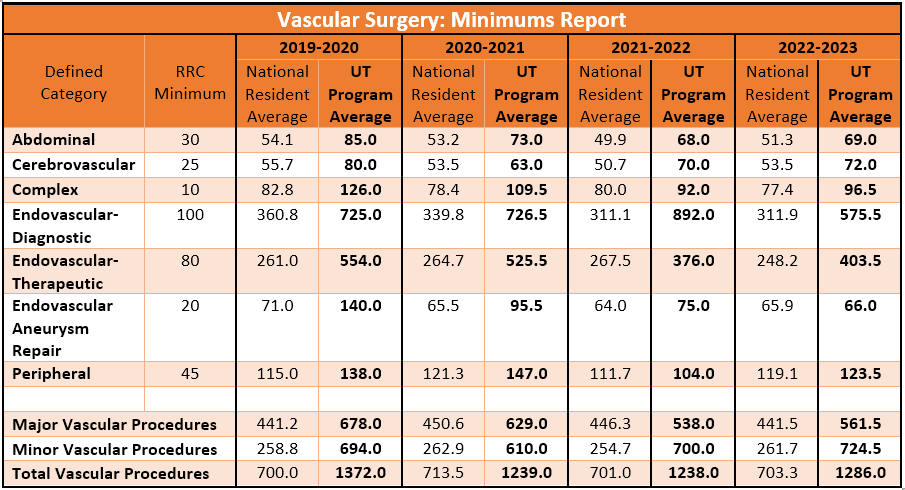
Defined Category and Minimums Report
2022-2023
2021-2022
2020-2021
2019-2020
2018-2019
2017-2018
2016-2017
The Aortic Center at the University of Tennessee Medical Center
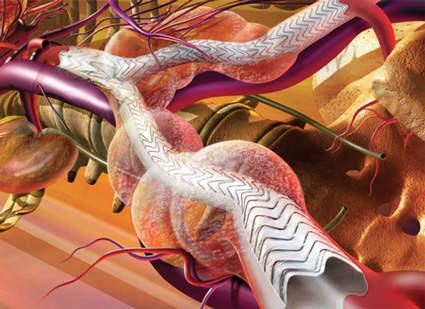 The Aortic Center at The University of Tennessee Medical Center is a regional referral center designed to provide easy and timely access for the evaluation and treatment of aortic aneurysm sand other abnormalities of the aorta. The center combines unique resources with experienced specialists that provide compassionate care to patients. Our team of surgeons and clinical staff work closely together to ensure the best possible treatment for patients. As the region's preferred hospital for the treatment of aortic disorders, the Center strives to set the standard for quality care.The Aortic Center provides unsurpassed leadership in the care of patients with aneurismal disease and trauma.
The Aortic Center at The University of Tennessee Medical Center is a regional referral center designed to provide easy and timely access for the evaluation and treatment of aortic aneurysm sand other abnormalities of the aorta. The center combines unique resources with experienced specialists that provide compassionate care to patients. Our team of surgeons and clinical staff work closely together to ensure the best possible treatment for patients. As the region's preferred hospital for the treatment of aortic disorders, the Center strives to set the standard for quality care.The Aortic Center provides unsurpassed leadership in the care of patients with aneurismal disease and trauma.
Learn More
Vascular Surgery Fellowship Programs
Program Fast Facts
ACGME Accredited: Yes
Fellows per year: 2
Application submitted through: Electronic Residency Application Service (ERAS)
Application Deadline: February 15th
Duration: 2 years
Postgraduate Training Required: General Surgery Residency, ABS/AOBS eligible
Salary Minimums: PGY6 $67,606
Benefits Include: Health and dental insurance, 15 days paid vacation, support for educational conferences
Contact Information

Michael M. McNally, MD
Program Director
Vascular Surgery Fellowship Program
Department of Surgery
Patty Hamilton, Fellowship Coordinator
Department of Surgery, Graduate School of Medicine
The University of Tennessee Medical Center
l924 Alcoa Highway, Box U-11
865-305-9006 or 800-596-7249
E-mail: phamilto@utmck.edu

(right to left) Dr. Michael McNally, (Program Director), Dr. George Lodeiro, Dr. Trent Kinnear, and Dr. Michael Freeman (Chairman)

Medical Simulation
Simulation is the imitation of real-life experience including the use of task and virtual reality trainers, as well as standardized patients to refine technical and clinical skills of healthcare professionals. At the UT Center for Advanced Medical Simulation, the goal is continual improvement in quality of patient care and safety through education, practice, and assessment. Simulation can replicate almost any diagnostic or therapeutic situation, from simple IV insertions using low-fidelity task technology to complicated surgeries using high-fidelity, computerized manikins or virtual reality modules.