Hord Award Honors Medical Students

![]() The UT Graduate School of Medicine recently awarded the Earl and Virginia Hord Endowed Scholarship to third-year UT Health Science Center College of Medicine students Kristen Campbell and Jennifer Wu. The Hord scholarship is a two-year award offered through the Graduate School of Medicine to COM students completing their full third and fourth years in Knoxville. The scholarship is given for demonstrated excellence in academics and requires a 3.0 GPA or above be maintained.
The UT Graduate School of Medicine recently awarded the Earl and Virginia Hord Endowed Scholarship to third-year UT Health Science Center College of Medicine students Kristen Campbell and Jennifer Wu. The Hord scholarship is a two-year award offered through the Graduate School of Medicine to COM students completing their full third and fourth years in Knoxville. The scholarship is given for demonstrated excellence in academics and requires a 3.0 GPA or above be maintained.
Both students said they chose Knoxville for their third and fourth years of medical school to take advantage of the smaller rotation sizes, allowing for more one-on-one time with attending physicians and residents. Campbell said, "We have the ability to directly interact with attendings and residents and not get lost in the crowd of students."
Campbell and Wu also both said they have support systems in Knoxville through family and friends, which can be a great advantage to providing balance to the demands of medical school.
Ultimately, the scholarship provides relief to the burdens of paying for school so that the students can focus on their education. Wu said, "I can't imagine how different my education would have been if it weren't for scholarships like Hord, and I'm all the more grateful that this exists."
Collaborative Radiology Study Improves PET Image Reliability
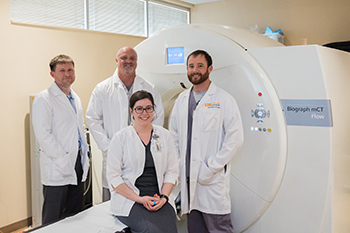 To have a PET scan, patients are injected with a radioactive sugar molecule that attaches to tumors. If the tracer does not attach properly, the scan may not produce reliable images, and a second scan may be needed. One reason the radiotracer does not attach is that is that it leaks into surrounding tissues — what doctors call "infiltration." Researchers at The University of Tennessee Medical Center are part of a nationwide quality improvement project led by Lucerno Dynamics to assess and reduce infiltration. Traditionally, infiltration is only confirmed if the injection site for the radiotracer is within the PET field of view. Even if the injection site is inside the field of view, the tracer may spread through tissue and not be visible on the images. However, Lucerno Dynamics has developed technology to assess injection quality, which ultimately helps radiologists determine the success of a scan and aids physicians in recommending the best treatment.
To have a PET scan, patients are injected with a radioactive sugar molecule that attaches to tumors. If the tracer does not attach properly, the scan may not produce reliable images, and a second scan may be needed. One reason the radiotracer does not attach is that is that it leaks into surrounding tissues — what doctors call "infiltration." Researchers at The University of Tennessee Medical Center are part of a nationwide quality improvement project led by Lucerno Dynamics to assess and reduce infiltration. Traditionally, infiltration is only confirmed if the injection site for the radiotracer is within the PET field of view. Even if the injection site is inside the field of view, the tracer may spread through tissue and not be visible on the images. However, Lucerno Dynamics has developed technology to assess injection quality, which ultimately helps radiologists determine the success of a scan and aids physicians in recommending the best treatment.
Through this quality improvement project, Dustin Osborne, PhD, Associate Professor of the Molecular Imaging and Translational Research Program, and his study team including nuclear medicine technologists in the Department of Radiology found their infiltration rates were 2.1 percent for the initial 10 week assessment period, among the lowest of the participating nationwide institutions.
Initial results from phase one of the study have indicated some areas where the team can focus to further improve the rate of infiltration which will be implemented later this year. The medical center has also been invited to participate in a follow up study that will compare the infiltration data to patient scans to determine whether a scan should be repeated based on reduced image quality.
Dr. Baljepally's Innovation Impacts Cardiac Care
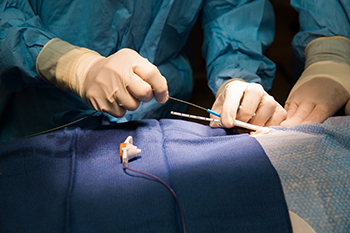
![]() Every day, physicians have to think on their feet. Sometimes, this quick thinking leads to game-changing techniques for the whole industry. This was the case when Raj Baljepally, MD, Clinical Assistant Professor of Medicine, and his medical team invented a new way of putting in a small heart pump, called an Impella device.
Every day, physicians have to think on their feet. Sometimes, this quick thinking leads to game-changing techniques for the whole industry. This was the case when Raj Baljepally, MD, Clinical Assistant Professor of Medicine, and his medical team invented a new way of putting in a small heart pump, called an Impella device.
The Impella pump sits in the left ventricle and is used to help hearts that are weak or failing to keep blood flowing to the body until the heart can recover enough to pump on its own.
Dr. Baljepally diagnoses and treats heart conditions with the help of tubes, called catheters. The catheters run from an artery in the groin or wrist into the heart. They send things like dye, or tools like the Impella, which help the medical team learn what is causing the heart to not function correctly, and to repair it when possible.
The Impella is used temporarily to keep the heart pumping until it can take over on its own. The catheter holding the device attaches to a machine at the bedside, which controls the pump. From that console the medical team can change how much the pump works. As patients recover, the team can turn down the pump and let the patient's own heart take over. Once that happens, the patient goes back into surgery and the doctors take the Impella out.
"This pump is a revolutionary method of management," said Dr. Baljepally. "You can keep blood flowing to the brain, kidneys and other organs during or after a procedure."
Dr. Baljepally and his team were working on a 45-year-old man who'd had a heart attack. They put a catheter through the patient's groin to his heart, then slid the Impella pump into place in the left ventricle. The Impella pump worked well for the first day, but as happens in a small percentage of patients, the wires of the pump kinked, which made the pump malfunction.
Scott Cook, MD, is a third-year Cardiology Fellow on Dr. Baljepally's team. He said, "When the pump stopped working, it made the patient's blood pressure crash. We knew we had to replace the pump."
The Impella pump is larger than the catheter that carries it to the heart. So when you take it out, the tube has to come out, too. This means, when the team needs to put in another device, they have to find a new place to put a catheter. The challenge is that heart patients are on high amounts of blood thinners. Using a second insertion site can cause the patient to bleed, which can be difficult to stop when the blood is so thin.
"But during this surgery," said Dr. Baljepally, "we found a new way to use the same site."
First, they took out the Impella and its catheter. Then, they placed a wire to hold open the site.
"We tried using the wire to thread in the new Impella, but the wire and the Impella's catheter together were too thick," said Dr. Baljepally. "So we discovered we could use the tubing of the Impella, itself, to slide a new catheter through," said Dr. Baljepally. "This let us put in a new device without endangering the patient with a second stick."
After the procedure, the team realized this information might be helpful for other medical teams. They went to the medical center's Simulation Lab and redid the procedure.
"We walked ourselves back through it step by step to figure out how to explain it to someone else," said Dr. Baljepally. "If other physicians learn to do this, it might help other patients, too."
Since then, Dr. Baljepally and Dr. Cook have published a paper in the medical journal, "Catheterization and Cardiovascular Interventions." As a result, the company that makes the Impella pump has started posting how-to instructions of the procedure on their consoles.
Our three part mission includes:

Regional and National News:
"UT Medical Center adds 5 new names to Wall of Distinction"
Knoxville News Sentinel
Featuring: Howard C. Filston, MD, Kimball Maull, MD, Vichien Lorch, MD
"How UT Medical Center became the region's leading trauma center"
WATE
Featuring: Kimball Maull, MD, Vichien Lorch, MD, Howard Filston, MD, Jack Lacey, MD
"Surgical Site Infections Successfully Curbed by Colorectal Bundle"
General Surgery News
Featuring: Brian Daley, MD
"UTMC leaning on medical experts to prept for disaster response"
WBIR
Featuring: Brian Daley, MD
"Wife's death led him to discover what may be a better breast cancer treatment"
USA Today
Featuring: Timothy Panella, MD
"Hard choices: UT research hints at better breast cancer treatment"
Knoxville News Sentinel
Featuring: Timothy Panella, MD
"Doctor's mission: Help opioid-addicted mothers, babies"
The Daytona Beach News-Journal
Featuring: Craig Towers, MD
"Dentists learn detective work at UT Body Farm"
WBIR
Featuring: Murray Marks, PhD
Faculty Awarded for Excellence
![]() Each year, faculty are recognized for their extraordinary efforts in education and discovery. The 15th annual University of Tennessee Graduate School of Medicine Faculty Awards were presented by James J. Neutens, PhD, Dean; William Metheny, PhD, Assistant Dean for Graduate Medical and Dental Education; and Mitchell Goldman, MD, Assistant Dean for Research, during the New Resident and Fellow Welcome Reception and Awards Ceremony. Faculty recognized for the 2017 faculty awards are
Each year, faculty are recognized for their extraordinary efforts in education and discovery. The 15th annual University of Tennessee Graduate School of Medicine Faculty Awards were presented by James J. Neutens, PhD, Dean; William Metheny, PhD, Assistant Dean for Graduate Medical and Dental Education; and Mitchell Goldman, MD, Assistant Dean for Research, during the New Resident and Fellow Welcome Reception and Awards Ceremony. Faculty recognized for the 2017 faculty awards are
 The GSM Spirit Award:
The GSM Spirit Award:
Amy Stevens, MD, Associate Professor, Family Medicine
In addition to associate professor, Dr. Stevens has been the Family Medicine Residency Program Director since 2007. She is noted for developing a program known nationally for producing well-rounded physicians. As faculty, she has earned her department's faculty teaching award twice and also won the GSM Excellence in Teaching Award in 2012. In leadership, Dr. Stevens completed the Physician Leadership Academy at The University of Tennessee Medical Center in 2013. She has also distinguished herself as a physician leader by serving on numerous committees at the medical center, most recently as a founding member of the Women in Medicine Organization. She has also been chair of the University Health Network; Chief of Staff in 2013 and 2014; chair of the Performance Improvement Committee; and many more. She has also served nationally as an academic council member for the National Institute of Program Director Development Fellowship and member of the Association of Family Medicine Residency Directors. She has published and presented numerous times and earned grants related to pulmonary research and a tobacco cessation project. Dean Neutens said, "Amy exemplifies the Graduate School of Medicine mission in healing, education and discovery with excellence, and we are grateful for her continued leadership not only in the Department of Family Medicine but also throughout the community."
 The GSM Spirit Award:
The GSM Spirit Award:
Amy Paganelli, MBA, CPA, Assistant Dean for Business and Finance
Dean Neutens honored Dean Paganelli with an honorary GSM Spirit Award, typically awarded to faculty only. He honored her for serving as his "right hand" for the past 10 years in all things related to finance for the Graduate School of Medicine. Through her oversite, she ensures the GSM support offices as well as the departments run smoothly so that the departments can serve the GSM mission. Dean Paganelli is responsible for all financial and budgeting aspects of the UT Graduate School of Medicine as well as administrative operations. She joined the graduate school in 1999 and served as Director of the UT Graduate School of Medicine's Office of Business Administration prior to being named Assistant Dean for Finance and Administration in 2007. Paganelli earned the Certified Public Accountant (CPA) designation in 1989. She serves on the Board of Directors of the local chapter of the Association of Government Accountants.
 Excellence in Teaching Award:
Excellence in Teaching Award:
Patrick McConville, MD, Assistant Professor, Anesthesiology
Dr. McConville has been with the UT Graduate School of Medicine since 2010 and currently serves as program director for the Anesthesiology Residency program. He has been selected by Anesthesiology residents to receive the department's faculty teaching award in both 2011 and 2014. Residents have commented that he is a huge resident advocate, pleasant to work with, makes himself available for teaching yet also provides a balance with autonomy. Dr. McConville is also an alumnus of the program. Robert Craft, MD, Chair of Anesthesiology, said, "Dr. McConville has distinguished himself in the area of resident education and his evaluations have been exemplary."
 Excellence in Teaching (Volunteer):
Excellence in Teaching (Volunteer):
Spencer Gregg, MD, Clinical Assistant Professor, Medicine
Dr. Gregg has been a volunteer faculty member with the UT Graduate School of Medicine since 2015. He has been serving as the medical director of the UT Student Health Center since 2010. In the student health center setting, residents are able to provide non-emergent, outpatient care to students and have access to specialty services such as laboratory and radiology, in addition to clinics in gynecology and surgery. Dr. Gregg also volunteered to host transitional year residents at a time when the program needed a rotation in an ambulatory setting. Rajiv Dhand, MD, Chair of Medicine, said, "Dr. Gregg is an excellent mentor to residents on their Student Health rotation. [His] lifelong commitment to learning is evident in his practice of medicine."
 Excellence and Leadership in Clinical Research:
Excellence and Leadership in Clinical Research:
James McLoughlin, MD, Professor, Surgery
Dr. McLoughlin has been with the UT Graduate School of Medicine since 2012 and conducts clinical research focused on surgical oncology. He has been principal investigator on several research projects, including the most recent on the evaluation of the role of ODAM in breast cancer and the role of ODAM in GIST tumors. He does research on healthcare policy and has helped form the relationship with the Haslam School of Business to generate a think tank on healthcare policy and new models for healthcare. Dr. McLoughlin actively also provided feedback to Senator Lamar Alexander regarding the revisions to the Affordable Care Act Healthcare Law. He serves on numerous committees both at the medical center and nationally. Bruce Ramshaw, MD, Chair of Surgery, said, "I have personally worked with Dr. McLoughlin on these efforts, and I can tell you firsthand his passion and commitment for improving healthcare is unmatched."
 Excellence and Leadership in Basic Science Research:
Excellence and Leadership in Basic Science Research:
Emily Martin, PhD, Assistant Professor, Medicine
Dr. Martin has been working in research at the UT Graduate School of Medicine since 2009 when she began as student volunteer. She developed a passion for studying amyloidosis and pursued a PhD through UT's Comparative and Experimental program. In 2014, she joined faculty as an assistant professor to continue her work to improve the lives of those who have amyloidosis. In 2016, she was awarded the Donald C. Brockman Memorial Research Grant for her project to evaluate a novel test for identifying patients who have multiple myeloma, or a similar disease, who are at risk of developing light chain (LC) amyloidosis. Also in 2016, Dr. Martin was instrumental in starting the first Amyloidosis Patient Support Group in East Tennessee. She has won numerous awards for best presentation and poster as well as travel awards at international imaging and amyloid-related scientific meetings.
Leadership Tennessee Selects Dr. Gray
![]() Keith Gray, MD, an Associate Professor and the Division Chief of Surgical Oncology, is also a self-described student of leadership, a focus that helped him gain a spot in the 2017-2018 Leadership Tennessee class.
It's highly competitive to become a member of Leadership Tennessee. First, candidates must be nominated. Once nominated, an anonymous selection committee chooses who will participate. For Dr. Gray's class, 300 people from all over the state were nominated. From that group, 42 were chosen. These leaders represent a variety of professional fields, including medicine, education and business.
Keith Gray, MD, an Associate Professor and the Division Chief of Surgical Oncology, is also a self-described student of leadership, a focus that helped him gain a spot in the 2017-2018 Leadership Tennessee class.
It's highly competitive to become a member of Leadership Tennessee. First, candidates must be nominated. Once nominated, an anonymous selection committee chooses who will participate. For Dr. Gray's class, 300 people from all over the state were nominated. From that group, 42 were chosen. These leaders represent a variety of professional fields, including medicine, education and business.
Dr. Gray has previously participated in Leadership Knoxville as well has helping to develop the Physicians Leadership Academy at The University of Tennessee Medical Center. He said, "When I started work as a physician, I had a lot of training and expertise in surgery. I didn't know I was a leader or had leadership potential, but the medical center recognized those abilities in me and encouraged me to develop them.
"Over time, I found that clinical skills don't necessarily translate into administrative skills. So I started looking for solutions, and out of that came the Physicians Leadership Academy. We partnered with the Haslam College of Business to teach doctors the business of medicine."
Through Leadership Tennessee, Dr. Gray hopes learn ways to make the medical center more well-known throughout the state, including by learning from other industries. "Outside of health care, other industries are doing things we can learn from," Dr. Gray said.
He also wants to help develop new programs at the medical center to help health care workers learn leadership skills. "The medical center has mentor and successor programs that prepare the next generation of leaders. In addition to the Physicians Leadership Academy, we're considering developing other leadership programs for staff and residents."
Dr. Scott Leads Interventional Cardiology Fellowship

![]() J. Christopher Scott, MD, is the new Director of the Interventional Cardiology Fellowship, following leadership by Dale Wortham, MD, who retired following a distinguished career. Interventional cardiology applies non-surgical techniques such as angioplasty and stenting to treat cardiovascular diseases. The Interventional Cardiology Fellowship at the UT Graduate School of Medicine is a one-year program designed to train physicians to become certified as a primary operator in Invasive and Interventional Cardiovascular Medicine.
J. Christopher Scott, MD, is the new Director of the Interventional Cardiology Fellowship, following leadership by Dale Wortham, MD, who retired following a distinguished career. Interventional cardiology applies non-surgical techniques such as angioplasty and stenting to treat cardiovascular diseases. The Interventional Cardiology Fellowship at the UT Graduate School of Medicine is a one-year program designed to train physicians to become certified as a primary operator in Invasive and Interventional Cardiovascular Medicine.
Dr. Scott said the one-person fellowship is like an apprenticeship in that the fellow gains expertise by practicing alongside seasoned subspecialists. Also, the subspecialty fellowship creates opportunities for medical learners at all levels, from medical students to Internal Medicine residents to general Cardiology fellows. "Even if residents are not planning to specialize in Cardiology, the fact that we offer this level of training says something very positive about the learning environment here," said Dr. Scott.
Dr. Scott received his medical degree from the UT Health Science Center in Memphis. He did both his internship and residency in Internal Medicine at Baptist Memorial Hospital in Memphis. He then completed a Cardiovascular Diseases Fellowship with UT. Dr. Scott has served as a Clinical Instructor and a Clinical Associate Professor of Medicine at the University of Illinois.
Dr. Gaylord Named UTHSC Outstanding Alumnus

![]() Mark Gaylord, MD, Professor and Director of Neonatology, was one of five distinguished alumni honored during the University of Tennessee Health Science Center' s (UTHSC) College of Medicine's Outstanding Alumni Awards luncheon. Dr. Gaylord completed his medical degree at UTHSC in 1978. His primary interest was in children's health, and he was named the Outstanding Pediatric Student by the college. His academic record was one of consistent excellence, resulting in membership in the Alpha Omega Alpha Honor Medical Society.
Mark Gaylord, MD, Professor and Director of Neonatology, was one of five distinguished alumni honored during the University of Tennessee Health Science Center' s (UTHSC) College of Medicine's Outstanding Alumni Awards luncheon. Dr. Gaylord completed his medical degree at UTHSC in 1978. His primary interest was in children's health, and he was named the Outstanding Pediatric Student by the college. His academic record was one of consistent excellence, resulting in membership in the Alpha Omega Alpha Honor Medical Society.
Following his graduation from UTHSC, he received a pediatric residency and neonatal-perinatal fellowship training at the University of Colorado Health Sciences Center, now known as the University of Colorado Anschutz Medical Campus. Upon completion, the University of Colorado immediately offered him a job as attending neonatologist and clinical instructor. After two years, he was recruited to join a burgeoning neonatal practice at the University of Tennessee, Knoxville.
Dr. Gaylord has worked for more than 30 years in the Newborn Intensive Care Unit (NICU) of the University of Tennessee Medical Center in Knoxville, and currently serves as the medical director for the NICU.
He is a tireless advocate, fighting the political battles for fair and equitable health care for all patients. In addition to his responsibilities as a clinician, Dr. Gaylord has been a professor for over 30 years. He is a full professor of pediatrics in the UT Graduate School of Medicine. He has been a member of the UTHSC College of Medicine's Knoxville campus faculty since 1986.
Dr. Gaylord is interested in new clinical research that could potentially benefit his patients. Two of his major contributions have been in developing a new type of incubator that improves the tiniest premature infant's microenvironment and working with the late Dr. Forrest Bird, inventor of the first baby ventilator, in developing one of the first high frequency ventilators. This new incubator is standard in most NICUs in the United States and the ventilator helped change the way babies with lung disease are treated.
Beyond his responsibilities for direct patient care and teaching, Dr. Gaylord has statewide responsibilities in administration through the Tennessee Perinatal Advisory Committee and Tennessee Initiative for Perinatal Quality Care. He has served important roles with the March of Dimes, the Ronald McDonald House, American Academy of Pediatrics, Healthy Families, Tennessee Perinatal Association and National Perinatal Association (for which he served as president from 2001-2002). He investigated and promoted the testing processes for detecting newborn hearing loss. These infant hearing tests are now part of the universal newborn screening in Tennessee and throughout the United States.
Dr. Gaylord has served as a member of the UTHSC COM Alumni Council since 2005, and he has been given the University Health System Philanthropy Award by the Great Smoky Mountain Chapter of the Association of Fundraising Professionals for his work on behalf of UTHSC.
Physicians Address Racial Disparities in Cancer
![]() The University of Tennessee Medical Center's Cancer Institute participated in the East Towne Health Fair on Saturday, September 9, hosted by Healthy Pathways, an initiative of the Beck Cultural Exchange Center and the Cancer Support Community.
The University of Tennessee Medical Center's Cancer Institute participated in the East Towne Health Fair on Saturday, September 9, hosted by Healthy Pathways, an initiative of the Beck Cultural Exchange Center and the Cancer Support Community.
This event was Healthy Pathway's first health fair and offered free health screenings, educational resources, fitness demonstrations, community resources, entertainment, and healthy lifestyle classes. UT Medical Center's Cancer Institute offered breast and prostate cancer screenings. Dr. Bedford Waters, Urology Chair, was in attendance at the event to perform prostate screenings.
Data shows that in Knox County, black men are more likely than white men to die of colon cancer. Black women are more likely than white women to die of breast cancer. Identifying and overcoming disparities like these is a goal of Healthy Pathways.
Dr. Keith Gray, Associate Professor of Surgery, has been involved with the initiative since it started to take shape at a 2015 forum. "For a really long time, we've kind of put (health) disparities into categories by race and ethnicity," Dr. Gray said. "As an African-American medical student, you begin to wonder, ‘Why does my race always do so much more poorly over all areas of health care?' ... The disparities exist along socioeconomic lines."
Dr. Gray and others have spent two years in Knoxville communities where disparities are highest, trying to learn why those communities have a higher risk of cancer and poorer outcomes and teach people how to decrease their risk of dying from cancer.
To learn more, read the recent Knoxville News Sentinel article by reporter Kristi Nelson at this link.
UTGSM Faculty Named to New University Health Network Board
![]() The inaugural Board of Directors for University Health Network (UHN) has been announced. UHN is a clinically integrated network formed by The University of Tennessee Medical Center and University Physicians' Association.
The inaugural Board of Directors for University Health Network (UHN) has been announced. UHN is a clinically integrated network formed by The University of Tennessee Medical Center and University Physicians' Association.
The intent of the network is to transform the care delivery system at the medical center to provide the right services for all patients at the right time, whether they are in the hospital, coming in for an outpatient visit, or following a care plan from home. It is a coordinated care plan that spans the entire episode of care.
"University Physicians' Association and The University of Tennessee Medical Center have had an excellent working relationship for nearly two decades now and this is the perfect illustration of how the two entities continue to move that relationship forward for our patients," said Amy Barger Stevens, MD, Associate Professor of Family Medicine and Chair of the UHN Board of Directors. "University Health Network provides a powerful collaborative construct through which both entities can provide the best quality, most efficient, patient centric care for the patients of our community."
The new board of directors includes 15 members, 12 of whom are physicians, with the majority of them being primary care physicians. This breakdown is carefully planned, as a clinically integrated network is driven by the primary care physicians on behalf of patients and their needs, regardless of whether they're coming in for a routine visit, are at home, or need to be hospitalized.
The Board of Directors are
Amy Barger Stevens, MD, (Chair), Family Medicine (Associate Professor)
Robert Elder, MD, UPA President (Professor)
Shelly Durbin, MD, Family Medicine
Crystal Gue, MD, Internal Medicine (Associate Professor)
Raymond Dieter, MD, Cardiothoracic Surgery (Professor)
Eduardo Mendez, MD, Internal Medicine
Jennifer Piel, MD, Internal Medicine
Clay Stalcup, MD, Family Medicine
Brian Daley, MD, General Surgery (Professor)
Amy Forsee, MD, Family Medicine
Rocio Huet, MD, Internal Medicine (Clinical Assistant Professor)
Jaclyn van Nes, MD, Obstetrics and Gynecology (Assistant Professor)
Joe Landsman, President and CEO, UTMC
Kim Friar, CEO, UPA
Steve Ross, Senior Vice President for Strategic Development, UTMC
Additionally, Julie Jeter, MD, Associate Professor, Family Medicine, will serve as Medical Director of UHN and Julia Coco is joining the medical center as Vice President of the clinically integrated network. Patients will be phased in to the network beginning next year.
U.S. News & World Report Names Medical Center as a Best Hospital

![]() The University of Tennessee Medical Center has earned recognition for the sixth consecutive year in the "Best Hospitals" edition of U.S. News & World Report. The 2017-2018 report ranks the medical center second in the state of Tennessee and as best regional hospital in the Eastern Tennessee region, based on its patient care performance and other key factors. Two adult care specialties at the medical center, Pulmonology and Nephrology, received national recognition, deemed by the publication as high performing services.
The University of Tennessee Medical Center has earned recognition for the sixth consecutive year in the "Best Hospitals" edition of U.S. News & World Report. The 2017-2018 report ranks the medical center second in the state of Tennessee and as best regional hospital in the Eastern Tennessee region, based on its patient care performance and other key factors. Two adult care specialties at the medical center, Pulmonology and Nephrology, received national recognition, deemed by the publication as high performing services.
The report additionally lists The University of Tennessee Medical Center as high performing in all nine of the Common Adult Procedures and Condition Ratings assessed in the survey:
- Abdominal Aortic Aneurysm Repair
- Aortic Valve Surgery
- Heart Bypass Surgery
- Heart Failure
- Colon Cancer Surgery
- Chronic Obstructive Pulmonary Disease (COPD)
- Hip Replacement
- Knee Replacement
- Lung Cancer Surgery
"Our physicians and team members recognize that we must continue to improve and advance our care capabilities daily on behalf of our patients and the community," said Joe Landsman, president and CEO of The University of Tennessee Medical Center. "It’s an honor to receive recognition in U.S. News Best Hospitals, because this highly credible independent assessment validates the compassion, care and talent of our outstanding healthcare providers and team members, as well as the contribution they make for those we serve."
James Neutens, PhD, Dean of the College of Medicine - Knoxville campus said, "The UT Graduate School of Medicine couldn't have a better clinical partner for our residency and fellowship programs."
Because of its independent analysis, the annual ranking by U.S. News is considered as an unbiased source for determining safety and quality in the medical field. Now in its 28th year, the Best Hospitals report recognizes hospitals that excel in treating patients facing the greatest health challenges. The information is designed to help patients make informed decisions about where to receive care for life-threatening conditions or for common elective procedures.
The rankings from the annual report were produced by U.S. News with nationally recognized research firm RTI International. The methodologies include risk-adjusted survival and readmission rates, volumes, patient experience, patient safety, quality of nursing care and other care-related indicators.
"For nearly three decades, we’ve strived to make hospital quality more transparent to healthcare consumers nationwide," said Ben Harder, managing editor and chief of health analytics at U.S. News. "By providing the most comprehensive data available, we hope to give patients the information they need to find the best care across a range of specialties."
For the 2017-2018 report, U.S. News evaluated more than 4,500 medical centers nationwide in 25 specialties. The "Best Hospitals 2018" guidebook is scheduled to be published in late August. Visit Best Hospitals for more information about the rankings.
