The Department of Anesthesiology
Curriculum
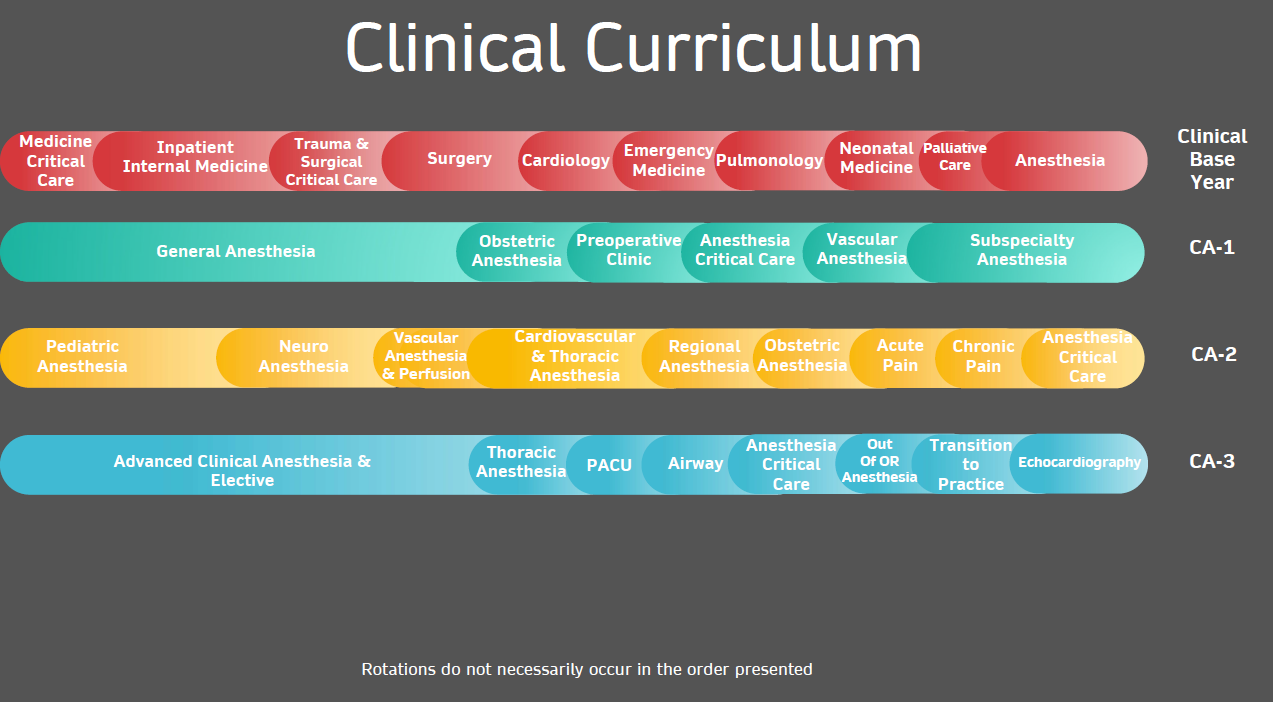
The Anesthesiology residency training program is a 4 year, categorical program, beginning with a Clinical Base Year.
Didactic Program
Resident education in anesthesia is supplemented by the expansive and rigorous reading and didactic program. Our program has had a great measure of academic success as evidenced by resident performance on in-training exams and American Board of Anesthesiology board pass rates. We strive to continually improve resident education by implementing changes to our didactic program based directly on resident feedback.

During the Clinical Base Year, residents are provided with textbook, Basics of Anesthesia, and are provided with an outline of recommended readings that correspond with various specialties through which they rotate.
| Presentation Topic Areas |
|---|
| Mock Orals |
Each resident in anesthesiology must complete a Mock Oral Examination in each of the Clinical Anesthesia years. At the beginning of each academic year, a case scenario and a faculty examiner are assigned to each resident. The resident uses information technology to locate and evaluate scientific studies, clinical recommendations and guidelines to incorporate into his preparation. On the assigned date, the examination proceeds according to a truncated version of the ABA Oral Board examination format, with the remaining members of the Department of Anesthesiology in attendance. At the conclusion of the examination period, a brief review of the resident’s responses ensues. |
| Problem-based Learning |
Each resident in anesthesiology must present a difficult clinical scenario to the Department of Anesthesiology in each of the Clinical Anesthesia years. A difficult clinical scenario will be assigned to the resident, who will be paired with a fellow resident and assigned a faculty mentor. The resident will use information technology to locate and evaluate scientific studies, clinical recommendations and guidelines to incorporate into his presentation. The resident will then utilize skills developed in part through the on-line educational module, The Resident as a Teacher, to educate the members of the Department of Anesthesiology (faculty and fellow residents) during this presentation at our monthly Problem-Based Learning Conference. This presentation will be led by the paired residents, and will include both a question-and-answer and lecture format. |
| Case Conference |
To aid residents in developing skills needed for the scholarship of dissemination, each resident is required to present a case conference during the CA-1 and CA-2 years. The resident, in conjunction with the faculty mentor, decides upon an interesting or difficult clinical case and presents challenges associated with the anesthetic management. As a requirement of the presentation, the resident is expected to use information technology to find, evaluate and incorporate data from the scientific studies for these presentations. |
| Morbidity & Mortality |
Residents are required to select and present a case for M&M during their CA-2 and CA-3 years. Each resident is expected to select a case in which they have not been involved and then identify what happened, present an analysis of the case with supporting literature and participate in an interactive discussion with the audience. |
| Root Cause Analysis |
Each resident must present one Root Cause Analysis (RCA), after having completed rotations in post-anesthetic recovery and pre-anesthetic assessment. Each resident is required to identify a problem, determine the basic underlying cause as opposed to merely 'treating the obvious symptoms.' During this exercise with the aid of a faculty mentor, the resident is expected to use the Six Sigma approach of repeatedly asking 'why' a problem occurs. By applying this type of methodology, the resident learns how to identify system errors and to suggest solutions. |
| Journal Club |
Journal Club occurs throughout the year with a goal of stimulating research hypotheses and updating clinical knowledge. These sessions take place during regular morning sessions, as well as special research-oriented evening sessions throughout the year. Residents work alongside faculty mentors to find articles from current general and subspecialty anesthesia journals that are relevant to the session's topic. Articles should be of research in nature. Residents choose one article for discussion and prepare slides to answer the questions via a PowerPoint presentation. |
| Grand Rounds |
Each CA-3 resident must present an hour-long Grand Rounds presentation about a clinically relevant topic of interest to the entire department. After discussion with the resident’s faculty mentor, a topic or interesting clinical case is selected. The resident uses information technology to locate and evaluate scientific studies to incorporate into his presentation. The resident then utilizes skills developed in part through the on-line educational module, The Resident as a Teacher, to educate the members of the Department of Anesthesiology (faculty, fellow residents, nurse anesthetists and student nurse anesthetists) during this presentation at our weekly Grand Rounds Conference. |
Simulation & Longitudinal Curriculum

Learn more about simulation at UTGSM.
News
Tweets by utgsm
Medical Simulation
At the University of Tennessee Center for Advanced Medical Simulation (UTCAMS), physicians, students, and other members of the healthcare team attain not only improvement in individual skills, but also learn and practice team skills that are essential for patient safety. This type of multi-faceted, orchestrated training improves critical thinking, decision making, and clinical techniques - all without imparting risk to a real patient. Discover how the UTCAMS is enhancing the learning of our anesthesiology residents and nurse anesthetists:
